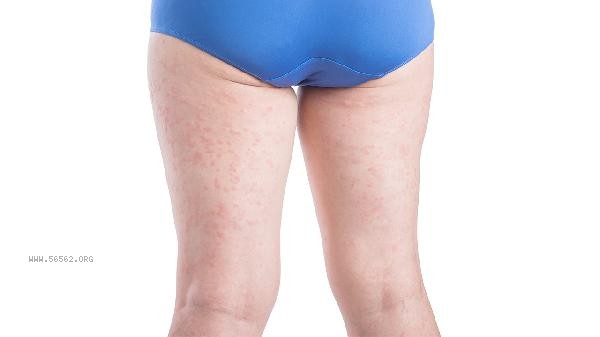
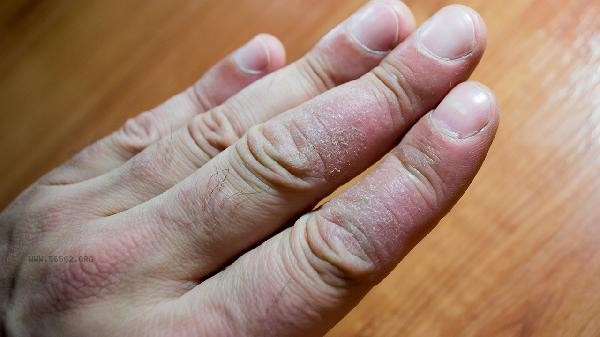
Abnormal coagulation function can lead to purpura on the skin. Purpura is a manifestation of subcutaneous or submucosal bleeding, which may be related to factors such as thrombocytopenia, coagulation factor deficiency, and vascular abnormalities. When coagulation function is abnormal, the hemostatic mechanism is impaired, and mild trauma or no cause can lead to skin purpura. Abnormal platelet count or function is a common cause of purpura. Thrombocytopenic purpura is characterized by skin petechiae and ecchymoses, which may be accompanied by nosebleeds and gum bleeding. Diseases such as immune thrombocytopenia and aplastic anemia can lead to thrombocytopenia. Treatment should be targeted at the primary disease, such as using recombinant human thrombopoietin injection, acetate prednisone tablets, and other drugs. In severe cases, platelet transfusion may be necessary. Lack or dysfunction of coagulation factors can also cause purpura. Hemophilia patients may present with joint cavity bleeding, deep tissue hematoma, and skin purpura due to a deficiency of coagulation factor VIII or IX. Vitamin K deficiency, liver disease, etc. can lead to insufficient synthesis of coagulation factors. Treatment requires the supplementation of corresponding coagulation factors, such as human coagulation factor VIII and prothrombin complex, while correcting underlying diseases. Abnormal vascular wall is another important mechanism. Allergic purpura, caused by the deposition of immune complexes, damages blood vessels and presents as symmetrical lower limb purpura, which may be accompanied by joint swelling and pain, as well as abdominal pain. Patients with hereditary hemorrhagic telangiectasia have increased vascular fragility, and slight collisions can lead to purpura. Treatment should avoid triggering factors, use vitamin C tablets and rutin tablets to improve vascular permeability, and in severe cases, use glucocorticoids.
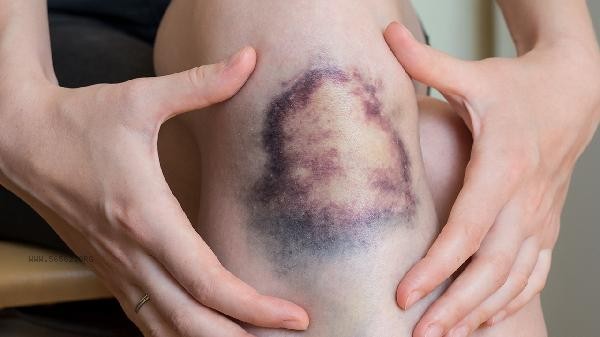
Other systemic diseases such as leukemia, disseminated intravascular coagulation, etc. may cause widespread purpura due to coagulation dysfunction. Leukemia patients have abnormal bone marrow hematopoiesis, reduced platelet production, and impaired function. Excessive consumption of coagulation factors during disseminated intravascular coagulation is manifested as multiple bruising and bleeding at the puncture site. Urgent treatment is required for primary diseases, such as acute promyelocytic leukemia induced differentiation with tretinoin tablets and arsenite injection. If skin purpura is found, seek medical attention as soon as possible to check blood routine, coagulation function, etc. Avoid intense exercise and trauma, and maintain skin cleanliness. A light diet is recommended, with moderate supplementation of citrus fruits and kiwis rich in vitamin C, as well as lean meat and animal liver rich in iron. Avoid using drugs such as aspirin enteric coated tablets that affect platelet function. Purpura accompanied by dizziness, vomiting blood, etc. requires immediate emergency treatment.









Comments (0)
Leave a Comment
No comments yet
Be the first to share your thoughts!