Diabetic patients can lose weight scientifically through diet control, proper exercise, drug assistance, blood glucose monitoring, behavioral intervention, etc. Diabetes combined with obesity may be related to insulin resistance, metabolic disorders and other factors, so it is necessary to develop individualized weight loss programs under the guidance of doctors.
1. Dietary Control
Adopt a low glycemic index diet, control the daily main food intake at 150-200 grams, and prioritize whole grains, legumes, and other coarse grains instead of refined rice and flour. The daily intake of vegetables should not be less than 500 grams, with dark vegetables accounting for more than half. Protein is mainly composed of high-quality proteins such as fish, shrimp, poultry, and soy products, with limited intake of saturated fats. Three meals can be adjusted to 5-6 small meals to avoid severe postprandial blood sugar fluctuations. Patients with combined kidney disease need to adjust their protein intake under the guidance of a nutritionist.
2. Moderate Exercise
Engage in 150 minutes of moderate intensity aerobic exercise per week, such as brisk walking, swimming, cycling, etc., with heart rate controlled within the range of (220 age) x 60% -70% during exercise. It is recommended to start exercising one hour after meals, with each session lasting 30-40 minutes. Cooperate with resistance training 2-3 times a week, focusing on exercising large muscle groups. Blood sugar should be monitored before and after exercise, and emergency candies should be carried to prevent hypoglycemia. People with retinal lesions should avoid jumping, holding their breath, and other movements.
3. Medication assisted
Metformin can be used as the first choice drug, which can improve insulin sensitivity and facilitate weight control. GLP-1 receptor agonists such as liraglutide injection can delay gastric emptying and increase satiety. SGLT-2 inhibitors such as dapagliflozin tablets reduce weight by promoting urinary glucose excretion. Avoid using hypoglycemic drugs that may increase weight, such as insulin secretagogues. All medication adjustments must be made under the guidance of an endocrinologist.

4. Blood glucose monitoring
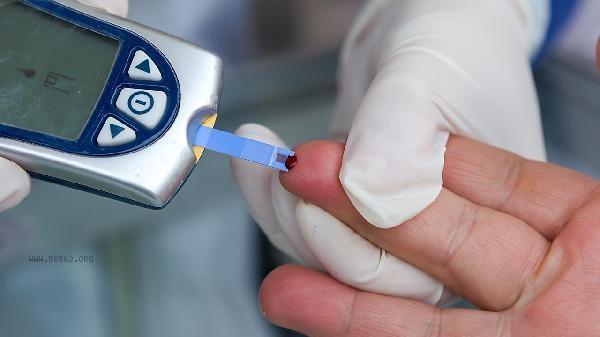
During weight loss, it is necessary to strengthen blood glucose monitoring and complete at least 7 fingertip blood glucose tests per day per week. Using a dynamic blood glucose monitoring system can provide a more intuitive understanding of the impact of diet and exercise on blood glucose. When the random blood glucose is below 3.9mmol/L or there are symptoms of hypoglycemia such as palpitations and sweating, 15 grams of quick acting carbohydrates should be consumed immediately. If blood sugar fluctuates excessively or hypoglycemia occurs repeatedly, seek medical attention promptly to adjust the plan.
5. Behavioral Intervention
Record daily diet and exercise diaries, and use the app to track weight trends. Set phased weight loss goals, typically aiming to lose 5% -10% weight within 3-6 months. Participate in diabetes health education courses and learn the calculation method of food exchange share. Seek family supervision and support to establish a regular schedule. People with anxiety and depression can seek help from a psychologist to avoid emotional eating.

Diabetic patients should lose weight at a constant rate of 0.5-1 kg per week. Rapid weight loss may induce ketosis. The daily water intake should reach 2000 milliliters and avoid sugary drinks. Regularly reviewing glycated hemoglobin and liver and kidney function, paying attention to changes in waist circumference is more meaningful than just weight alone. If there is obvious weakness, blurred vision or other discomfort, timely follow-up is needed. Maintaining a healthy lifestyle in the long term is more important than short-term weight loss, and requires the joint cooperation of medical teams, families, and patients.








Comments (0)
Leave a Comment
No comments yet
Be the first to share your thoughts!